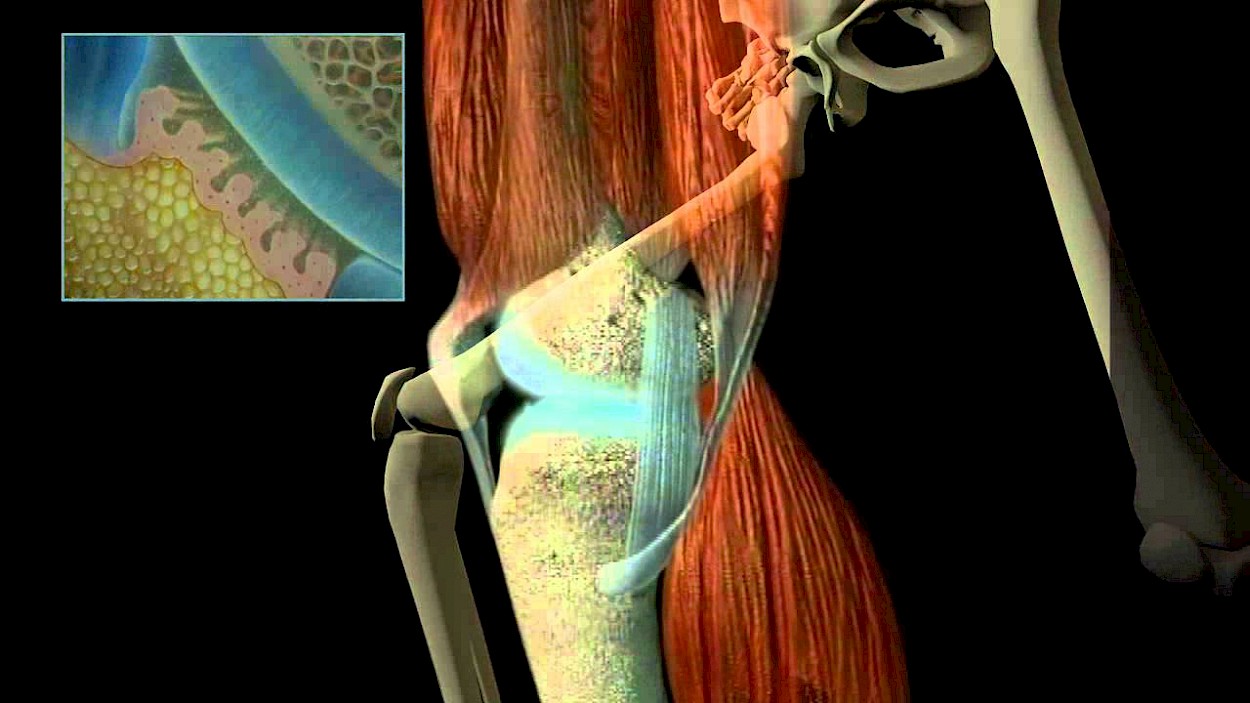
Osteoarthritis | Cartilage Damage
Risk factors for osteoarthritis include:
- Obesity
- Deformity of the joints (for example-back or legs)
- Sports with a higher rate of injury (e.g., soccer, skiing)
- Occupations involving lifting or carrying heavy loads
- Inactivity, such as lack of exercise
What are the symptoms of osteoarthritis/degenerative joint disease?
The first signs of osteoarthritis or degenerative joint disease are often the so-called "start-up pains" in the affected joint that occur after prolonged sitting or lying down, but improve after the affected joint is moved. With the progression of osteoarthritis, the movements of the joint become increasingly more painful. Certain movements may cause grating or grinding sound in the joint and/or the mobility of the affected joint(s) may be limited. In the last stage of osteoarthritis, the affected joint(s) will also ache during resting periods. Inflammation and swelling in the joint(s) can occur at any stage of osteoarthritis.
Treatment options for osteoarthritis/degenerative joint disease
Basically, the treatment of degenerative arthritis / osteoarthritis depends on the extent of joint deterioration and the patient’s level of expectation. The treatment strategy for a 30-year-old should certainly be different than that for an 80-year-old person. However, in all cases, it is mandatory that the treatment should be as gentle and gradual as possible. The first step will be to try a conservative, non-surgical therapy. A major component of conservative therapy is the treatment with hyaluronic acid. Only if this does not lead to long-term success, surgical treatment should be considered. Below is an overview of the basic conservative treatment options for osteoarthritis/degenerative arthritis.
Conservative treatment options for osteoarthritis/degenerative arthritis:
- Avoiding/correcting the above named risk factors, if possible
- Physiotherapy (physiotherapy, manual therapy, osteopathy)
- Physical measures (cooling, ointments, curd envelopes, herbal agents)
- Pain relievers (Paracetamol)
- Anti-inflammatory drugs, e.g. Ibuprofen, Diclofenac, etc. taking into consideration possible risks and side effects
- Physiotherapy
- Cortisone injections (including any risks and side effects)
- Hyaluronic acid injections
- Injections with Autologous Conditioned Plasma (ACP)
Alternative treatment options for osteoarthritis/degenerative arthritis
- Homeopathic remedies (for example, arnica compound, Traumeel)
- Dietary supplements (glutamine sulfate; chondroitin)
- Magnetotherapy
- Acupunkture
- Neural therapy
Hyaluronic acid treatment – what should you know?
Musculoskeletal System / Joint structure
Among the most important parts of a joint is the articular cartilage that covers the ends of the bone. With its smooth, durable substance, the cartilage provides a better gliding mechanism and shock absorption.
The joint is provided stability by the tight but very elastic capsule – the joint capsule, but also by the surrounding muscles. The joint capsule is lined by the mucous membrane, the so-called synovial membrane and completely encloses the space around the joint surface. The mucous membrane provides the joint with a viscous fluid called synovial fluid, or "joint lubricant".
When the joint is moved, the synovial fluid (synovial fluid) is evenly distributed throughout the joint space, and thus also on the cartilage surfaces. It is the main nourishing source for the cartilage since it contains no blood vessels.
Only a good nutrition situation of cartilage ensures sufficient elasticity and its resistance to abrasion and wear. In addition to the nutrients for the cartilage, the synovial fluid contains another very important ingredient, namely the hyaluronic acid. The hyaluronic acid is responsible for the consistent lubrication with synovial fluid. The hyaluronic acid has a similarly important function as the oil in the engine and the transmission of a car
How does artificial hyaluronic acid work?
In osteoarthritis, the synovial fluid is subject to decisive changes. Normally, the synovial fluid functions in finely tuned balance between the old hyaluronic acid degrading and a new hyaluronic acid being proded.
In osteoarthritis, this balance is disturbed and the result is an inferior too "thin" joint fluid. As a result, it loses some of its beneficial properties, namely lubrication and shock absorption are no longer sufficient and cannot protect the joint against abrasion and wear. The articular cartilage is worn away and gradually loses its elasticity. As a result, the cartilage becomes less resilient, and does not sufficiently fulfill its protective function for the underlying bone structure. Once destroyed, cartilage tissue cannot regenerate itself, meaning it cannot heal.
Synthetic hyaluronic acid can be injected in between the spaces of the joint for the improvement of the joint's synovial fluid. Here it supports the body to restore the natural balance between degenerating and regenerating the synovial fluid. The joint’ synovial fluid turns viscous again with the help of the injected hyaluronic acid and can thereby improve its lubricating protective effect. The joint’ synovial fluid turns viscous again with the help of the injected hyaluronic acid and can thereby improve its lubricating protective effect. The articular cartilage is relieved by the protective hyaluronic acid layer. The wear does not continue disproportionately. Joint mobility is improved and pain subsides.
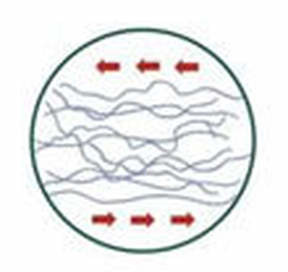
Fig. 1 With equally distributed stress, hyaluronic acid acts as a lubricant
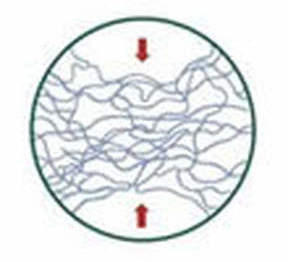
Fig. 2: Under sudden stress the hyaluronic acid acts as a shock absorber
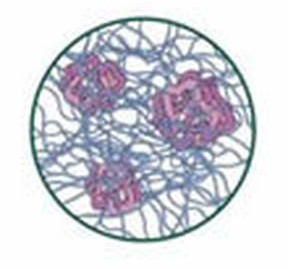
Fig. 3: The hyaluronic acid functions as a filter restricting the passage of harmful molecules and cells into the joint space
How often should the affected joint be treated with hyaluronic acid?
Depending on the joint, and the severity of the osteoarthritis, injections with a highly concentrated hyaluronic acid are administered three to five times into the affected joint. The injections should be given once a week
Although the body degrades the injected hyaluronic acid, it has been shown that its effect lasts a long time. This is explained by the fact that the substitution treatment with hyaluronic acid stimulates the body's own production of hyaluronic acid. With milder cartilage damage often a single injection series of 3 to 5 syringes is sufficient to relieve the symptoms permanently. In moderate cartilage damage, injections should be repeated at intervals of every 12 months. In advanced osteoarthritis, the injections can be more frequent, i.e. may be administered every six months.
How is the hyaluronic acid therapy evaluated scientifically?
In recent years, in addition to medication and physical therapy, the use of hyaluronic acid has been established as part of the treatment of osteoarthritis. Meanwhile, the hyaluronic acid treatment of national and international professional societies has been included in the treatment of osteoarthritis treatment recommendations.
The DGOOC (German Society of Orthopedic Surgery) Guidelines classify systemic slow acting drugs, which also include hyaluronic acid, along with the symptomatic therapy such as NSAIDs, as first level therapy. In addition, the task force of the EULAR (European League against Rheumatism) has included hyaluronic acid in the recommended therapy management. Furthermore, the current Cochrane review also confirmed that intra-articular hyaluronic acid is an effective and useful treatment of osteoarthritis, especially in terms of the parameters pain, function, and general assessment by the patient. The analysis covered 17 different hyaluronic acid products. A total of 63 studies were analyzed
What alternative treatments other than a hyaluronic acid therapy are available for the treatment of osteoarthritis/degenerative arthritis?
Whether the treatment of cartilage damage with hyaluronic acid is meaningful, what the risks are, and how successful the treatment can be, should be discussed individually with the patient after the necessary examination(s) have been carried out and a diagnosis is available.
Specialists: Osteoarthritis / Degenerative Arthritis
For an optimal treatment of osteoarthritis/degenerative arthritis/degenerative joint disease, the knee experts at the Klinik am Ring are particularly well-qualified. Stefan Preis, M.D. and Jörg Schroeder, M.D., senior physicians at the Practice and Department of Orthopedics and Sports Traumatology at the Klinik am Ring in Cologne, specialize together with their team in the treatment of knee and shoulder disorders. In 2004, they founded the WEST GERMAN SHOULDER KNEE & CENTER, Cologne. The team consisting of eight specialists, treats more than 10,000 patients each year with joint diseases and disorders, whereby the treatment of osteoarthritis is of primary concern.