
„Top 5“-Diagnoses for Shoulder Pain

PDF Download
During recent years, physicians and physiotherapists have observed that the number of complaints in the area of the shoulder has increased and is still increasing. Due to the changing leisure habits and the rightly claim of the population to even in a mature age live an active life style, shoulder pain are increasingly moving into the focus of medical care. The causes of shoulder problems are manifold. It is therefore of utmost importance to establish an accurate diagnosis at the early stage of a shoulder disorder or disease. Only a timely diagnosis allows for an effective treatment.
Below, we would like to introduce the "Top 5", i.e. the five most common conditions that may be responsible for shoulder pain, their diagnosis and appropriate treatment options. As always, we favor the pragmatic approach "From the practice, for the practice."
Common causes of shoulder pain
Primarily responsible for shoulder pain are
- Impingement-Syndrome
- Calcific Tendenitis
- Rotator Cuff Rupture
- Adhesive Capsulitis/Frozen Shoulder
- Acromioclavicular joint osteoarthritis
Certainly the medical and therapeutic practice may not ignore the numerous differential diagnoses, particularly diseases and disorders of the cervical spine, as well as osteoarthritis, rheumatoid arthritis, tumors, internal diseases, neurogenic diseases, functional disorders, tendonitis, bursitis, traumatic injuries, instabilities and other diseases.
Impingement Syndrome – Shoulder
Synonyms: shoulder tightness syndrome, subacromial narrowness syndrome, periarthritis humeroradial scapularis (PHS)
Definition and Etiology
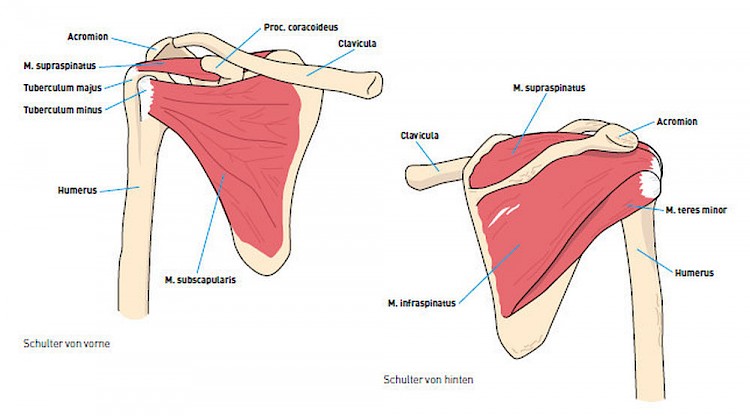
An impingement syndrome is characterized by shoulder pain that develop due to the narrow space between the acromion process of the scapula and the head of the humerus. Since by nature, a certain narrowness exists already in this region, further narrowness can lead to chronic irritation of the tendon (supraspinatus / rotator cuff) and the bursa. For the lateral lifting of the arm above 60 °, which is painful in an impingement syndrome, primarily responsible is primarily the supraspinatus muscle Acute or chronic compression or frictional loads to the rotator cuff are the cause of the impingement syndrome. Accordingly, the disease occurs frequently in sports, due to increased overhead activities, tennis, volleyball or throwing or even in professions with artisans such painters.
Diagnosis
Case history
The patient complains mostly about pain in the shoulder and in the proximal humerus during lateral raising the arm above 90°. Especially pronounced is the pain in abrupt movements or under stress. However, a patient's history also often indicates pain during resting and sleeping periods.
Clinical features
On examination, the shoulder indicates in most cases few or no findings. Passive, the shoulder can usually moved freely (170° flexion, abduction 90°, internal / external rotation 70/0/90°). The function tests painful-arc, Hawkins- and Jobe test are usually very positive, e.g. painful.
Impingement-Test
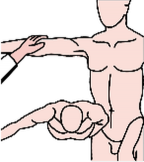 Jobe Test: provocation test for the evaluation of the supraspinatus. Procedure: active elevation of the arm against resistance from 90° abduction with inner rotating arm. If there is pain and / or loss of strength, the Jobe test is considered positive. It is an indicator for a subacromial impingement, and with decreased strength, it indicates a rupture of the supraspinatus.
Jobe Test: provocation test for the evaluation of the supraspinatus. Procedure: active elevation of the arm against resistance from 90° abduction with inner rotating arm. If there is pain and / or loss of strength, the Jobe test is considered positive. It is an indicator for a subacromial impingement, and with decreased strength, it indicates a rupture of the supraspinatus.
Imaging diagnostics
Ultrasound: to assess the subacromial bursa, the rotator cuff and the evaluation of a possible joint effusion.
Radiology: shoulder in three levels (ap / aro, ap / iro, outlet view / Y recording) to assess the bony relationships (hook acromion, increased lateral acromion slope, arthritis, calcific tendinitis).
MRT: comprehensive information on all bone and soft tissues of the joint structures, especially in cases of suspected rotator cuff and to assess the inflammatory condition.
Conservative Therapy
Resting the shoulder
The most important measure should be to avoid movements that cause pain, such as stressful and repetitive movements. This means to rest the shoulder, e.g. to refrain from sport activities that stress the shoulder and accordingly to avoid occupational, stressful shoulder movements.
Medicinal treatment
Recommended are non-operative measures such as a medicinal therapy, e.g. orally administered NSAID (diclofenac 2 x 75 mg / d or ibuprofen 3 x 600 mg / d for two to three weeks). An alternative is a local infiltration treatment of subacromial space, i.e. injections peritendinous into the subacromial bursa. In the acute phase e.g. triamcinolone 10 mg and dexamethasone 4 mg in 10 mL bupivacaine 0.5% (Caution with corticoids: time between two injections should be at least 4 weeks, with a total of no more than three repeats!). In chronic cases, if necessary, 1 Amp. Traumeel on 10 ml bupivacaine 0.5% six times at weekly intervals. Regarding joint injections we refer to the recommendation of the German Society of Orthopaedics and Traumatology (DGOU).
Physiotherapy
Physiotherapy aims at compensating muscular imbalances where by the focus is on achieve a relieving subacromial space gain in the shoulder, which requires that the humeral head ascending muscles must (supraspinatus, deltoid) detonisiert and the humeral head descending muscles (external rotators: infraspinatus, teres minor, rotators: subscapularis) are strengthened. Especially helpful and efficient are instructions to guide the patient to exercise independently. Locally administered measures that activate the metabolism are cross friction, ultrasound, electric or cryotherapy. They promote the regeneration process of the tendon tissue.

Shockwave therapy
Shockwave therapy is an alternative treatment for chronic painful tendon irritation, especially when classic conservative treatment measures such as medication, physical therapy, etc. do not lead to a lasting relief of the symptoms. Targeted shock wave therapy increases the metabolic activity is induced into the tendon injury. Due to the improved metabolism of otherwise bradytrophic tendon tissue, the capability of natural regeneration will be increased. As a rule, three treatments are carried out at intervals of one week, each, whereby 2,000 to 2,500 pulses are applied at a frequency of approximately 7 Hertz.
Surgical treatment
If shoulder complaints persist despite consistently conservative treatment over 3 to 4 months or if there is recurrent, stress-related complaints, operational measures should be considered. This allows the impingement syndrome to be treated causally and chronic tendon damage, possibly even a threat of rotator cuff rupture can thus be prevented. Such surgical procedure is referred to as "subacromial decompression".
Arthroscopic subacromial decompression can be done stationary (1 to 2 nights) or possibly even on an outpatient basis. Postoperatively the arm must be resting the first 4-6 weeks. Immobilization is not required. Physiotherapy treatments should accompany the recovery process. With proper indication and if performed by an experienced surgeon, arthroscopic subacromial decompression shows excellent results. In arthroscopic procedures, the surgical risk (infection, wound healing, etc.) is very low.
Calcific tendinitis
Synonyms: Calcified shoulder
Definition and Etiology
Calcifying tendinitis is a local deposition of calcium crystals in the rotator cuff. It mainly affects middle-aged women and men. The etiology of calcific tendinitis is not entirely clear. The primary theory is that locally restricted oxygen nutrition of certain tendons areas appears to be responsible. However, also discussed are causes like repetitive micro traumatizations, in connection with a subacromial impingement. Can be divided into three stages. The pre-calcification, the calcification and the post-calcification. ... The post-calcification stage is followed by the resorptive phase, which eventually ends up in a restitutio ad integrum with spontaneous dissolving of the calcium deposit.
However, the resorption of the calcium deposit can also fail, only incomplete or it can be interrupted temporarily. This can lead to symptomatic persistence of the calcium deposit, possibly also lead to a so-called post-calcification tendinitis with ongoing shoulder problems despite radiological evidence of complete resorption of the calcium deposit.
Symptoms
The symptoms of calcific tendinitis are highly variable. They range from asymptomatic conditions to slight motion-dependent complaints, to more or less strong pain while resting, to hyperacute pain. This massive pain often occurs during the partial penetrating of the calcium deposit into the subacromial bursa.
Diagnosis
Case history
DThe history is quite unspecific. Most of the patient complains of shoulder pain radiating into the anterolateral humerus.
Clinical examinations
Clinical examinations are highly variable depending on the size and location of the calcium deposit. A large calcium deposit, especially in the supraspinatus tendon, is often indicated by a limited motion, which cannot be overcome or only with considerable pain.
This often leads to evasive movements and apparent movement restrictions, which over time also become painful even at slight modifications of the direction the arm is moved. In extreme cases, the examination of the shoulder pain is almost not possible (resorptive phase).
Imaging Diagnostics
Sonography: On suspicion of calcifying tendinitis, sonography is a simple and reliable diagnostic method. The calcification is shown as sickle-shaped structure within the rotator cuff with typical acoustic shadow.
Radiology: The most sensitive imaging method for calcific tendinitis are radiographs in beam direction in external and internal rotation as well as the „outlet view" projection. Here it is possible to classify a calcium deposit due to its Radiology morphological properties (Gardener classification) and its development.
MRI: Magnetic resonance tomography is only of minor importance in the diagnosis of calcifying tendinitis.
Therapy
In our view, in most cases conservative treatment should be tried for at least six months. Regarded as negative prognostic factors for the success of a conservative therapy is the localization of calcification in the supraspinatus tendon and a large volume of the calcium deposit.
Conservative Therapies
The therapeutic measures for chronic complains due to calcific tendinitis are largely similar to those in subacromial impingement. The previously-held hope to crash/dissolve a calcium deposit in the rotator cuff with shockwave treatment, similar stones in the kidney, has according to the current studies not been successful. Therefore, the shockwave treatment does not belong to our standard treatment of calcific tendinitis.
In acute or peracute calcific tendinitis the patient experiences violent shoulder pain due to the dissolving of the calcium deposit in subacromial bursitis. In addition to immobilization and cooling high dosed oral anti-inflammatory drugs (2 x 75 mg/d or ibuprofen 3 x 800 mg/d, e.g. diclofenac), in combination with analgesics, e.g. novaminsulfon / metamizole are necessary. If these medications are not sufficient, local infiltration into the subacromial space, e.g. into the bursa with 40 mg and dexamethasone 0.5%., triamcinolone 8 mg to 10 mL bupivacaine should be considered. If it comes to complete resorption of the calcium deposit, the disease calcific tendinitis is cured. If there is only partial resorption of the calcium deposit, the inflammations might flare up repeatedly.
Surgical treatment
If complaints persist despite conservative therapy surgical, arthroscopic removal of the calcium deposit is indicated. Here, the regular pathologically altered bursa of calcium is first removed subacromial, a longitudinal incision is made over the tendon, and in addition the area is cleaned by lavage. In pasty calcium deposits this quite easily achieved. If the calcium deposit is of a more crystalline texture, a complete removal of calcium deposits should not be forced at the expense of the rotator cuff. In such cases the tendon is needled instead. Here, the tendon is punctured several times with a needle up into the bone and thus a "healing response" is induced, e.g. As part of the healing process the calcium deposit will be diminish gradually due to the increased circulation. Still detectable remains of calcium deposits immediately after surgery, therefore have a high spontaneous resorption rate. In existing impingement, arthroscopic calcium removal should be combined with an arthroscopic subacromial decompression. The treatment results are medium and long term in 90% of the cases very good. Recurrences are not expected.
Rotator Cuff Rupture
Synonym: Tendon Tear Shoulder/Ruptured Tendon
Etiology
The tendons surrounding the shoulder may tear as a result of an acute injury such as an accident or a fall on the arm or may be caused by chronic wear and tear with degeneration of the tendon. Mostly, however, pre-existing, chronic degeneration of the tendon is the main reason for a tendon rupture. With a previously damaged tendon, even everyday activities can sometimes be sufficient to cause a partial or complete tear. Predisposing for a rotator cuff tear is a chronic subacromial impingement. Especially n the supraspinatus tendon is often affected by a rupture. In old age, there are frequently asymptomatic ruptures of the rotator cuff
We differentiate between partial and complete tendon ruptures. In a so-called partial tendon rupture, the soft tissue is damaged, but not completely severed, while in a complete tear, the entire tendon (full-thickness tear) is ruptured splitting the soft tissue into two pieces. A partial tendon rupture has a general tendency to progress into a full-thickness tear. Likewise, even a complete tendon rupture tends to worsen when the cause is not addressed.
Case history
In an acute injury to the rotator cuff, the person concerned complains of sudden, often stabbing pain, especially when moving the arm upwards. Frequently, the function, in particular the strength of the arm is noticeably reduced. Because of a developing inflammation, frequently chronic nighttime shoulder pain radiates regularly into the upper arm.
Clinical Examinations
On examination, the shoulder is in most cases not very conspicuous. Passive the shoulder is usually freely rotated (170 ° flexion, abduction 90°, internal / external rotation 70/0/90 °), but usually indicates a more or less strong pain.
In particular, specific provocation tests for each tendon section are important for a differential diagnosis. If there is a rupture of the supraspinatus tendon, lifting the arm sideward (painful arc) or forward (Jobe test) is painful and strength is decreased. If there is a rupture of the infraspinatus tendon (optionally in combination with damage to the teres minor) the external rotational force is weakened or painful. In tendon rupture of the subscapularis internal rotation force of the arm is likewise weakened or painful (lift-off test).
Image Diagnostics
If a rotator cuff tear is suspected, targeted instrumental tests such as ultrasound or MRI are strongly indicated for the presentation of the tendons. The MRT is certainly the more comprehensive information and is essentially mandatory for suspected rotator cuff tear.
Therapy
Fact is that a torn rotator cuff has no self-healing tendency, whereby, the tear is, nevertheless chronically progressive. The decision here is whether with conservative treatment measures, despite a torn tendon, a functional, pain-free or pain-poor shoulder joint can be expected long term or whether this damage at the shoulder should be repaired surgically. All treatment strategies are generally based on the individual symptoms, the patient’s expectations and individual life style. In young patients or physically very active people, a tendon reconstruction, e.g. suturing the tendon, should generously be done even in case of a smaller tear. Simultaneously, a possibly existing impingement must be eliminated. The lower the patient’s expectations on motion and strength, e.g. as in elderly people, the more conservative the reconstruction of a ruptured tendon. In such cases, quality of life can possibly be restored even with conservative therapy measures.
Conservative treatment
The aim of a conservative therapy for an injury of the rotator cuff is to relieve the pain symptoms and functional deficits, e.g. reduce loss of muscle function at the arm and to reduce the risk of the damage progressing. A very important measure is that the patient avoids movements causing pain and straining the shoulder.
The conservative treatment of a rotator cuff rupture basically does not differ significantly from the therapy for an impingement syndrome. However, shock wave treatment should be excluded.
Surgical treatment
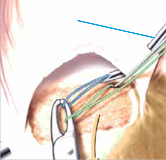
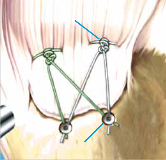
Today modern shoulder surgery offers the possibility to treat tendon tears within the scope of arthroscopic procedures. With the arthroscopic surgical technique used by experienced shoulder specialists torn tendons can today be repaired in such an effective way as was previously in open, also very traumatic surgeries not possible.
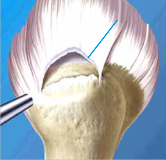
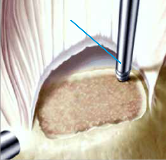
For the reconstruction, the torn tendon ends are reattached to the bone using small suture anchors (titanium, peak or bioresorbable materials), so that they can firmly heal at the bone. Simultaneously, it is generally necessary to expand the space below the acromion to protect the tendon against unnecessary pressure load and to ensure their healing.
The fresher and smaller a rotator cuff tear, the better the chances of recovery. Extensive ruptures that might exist for months require special skill and operational experience to achieve success. If a reconstruction is no longer possible, the focus lies on a smoothing of the torn tendon stumps and removal of the inflamed tissue. Only in exceptional cases is an elaborate reconstruction through shifting tendons of other muscles (latissimus dorsi transfer) meaningful.
Complex ruptures of the rotator cuff that cannot be reconstructed and cause excessive pain, may require the implantation of an inverse shoulder prosthesis.
Postoperative treatment
For the tendon to heal properly to the bone after a rotator cuff repair, it needs rest. To assure appropriate healing, the shoulder is first protected with a sling for three to six weeks. It is highly recommended to start intensive physiotherapy as a part of post operative treatment. Initial post-operative drainage is indicated. For the prophylaxis of a frozen shoulder, the joint must be passive mobilization as early as possible. Gentle isometrics exercises in the neutral position of the shoulder are to prevent an increased muscular atrophy. Accompanying muscular imbalances, particularly tension in the cervical spine, must be compensated. Targeted muscle training can be started after a minimum of 6-8 weeks after the surgery. During postoperative treatment it is important to include the patient in the treatment plan and to provide guidance for exercising on his/her own.
Adhesive capsulitis
Synonyms: frozen shoulder, stiff shoulder
Definition and Etiology
Adhesive capsulitis most often referred to as frozen shoulder, is a benign disorder characterized by shoulder pain and a reduction in active and passive mobility. It is tedious with disease duration of 12 to 36 months and has a phasic course. The entire process is often self-limiting and incomplete restitutions occur. Differentiated are primary and secondary forms. In primary frozen shoulder, the etiology is unknown, frequencies associated with metabolic disorders (diabetes mellitus, thyroiditis) are described. The secondary form triggers based mechanical damage, injury or surgery usually preceded. Morphologically Adhesive capsulitis yields a reduced volume in the joint cavity and synovitis. Histological there is a fibrotic capsule.
Diagnosis
Adhesive capsulitis can often be found on the basis of the patient’s medical history and clinical examinations. However, especially at the beginning, these are often non-specific.
Case history
In the early phase the patient complains about shoulder / arm pain that occurred for no apparent reason radiating into the upper arm that. Usually, there is remaining pain, but also motion-dependent pain. Over time there is increasing stiffening of the shoulder.
Clinical features
Clinical examination shows in case of a primary and secondary frozen shoulder three stages, each stage lasts an average 4-8 months. Stage I (freezing phase) is characterized by initially nonspecific progressive pain and is associated with an increasing restriction of movement of the shoulder. In Stage II (frozen phase) the inflammation and with it the pain resolve, however, the movement restriction initially continue. In Stage III, the resolution phase (thawing phase), the restriction of movement goes back and the mobility of the shoulder increases.
Imaging diagnostics
X-ray examination shows no pathognomonic indications of capsulitis - osteoarthritis is ruled out as differential diagnosis. In ultrasound we often find non-specific accumulation of fluid in the bursa, intra articular and the sulcus bizipitalis, indicating the inflammatory stage. Magnetic resonance imaging does however provide discreet hints especially in the inflammatory phase I, It allows for the differentiation between primary and secondary capsulitis. In the T2-weighted images a liquid equivalent correlate and a joint effusion in the area of the caudal recess can frequently be identified.
Therapy
Treatment of adhesive capsulitis is initially conservative. Only if this fails after a 3 to 4 months therapy, surgical treatment is indicated.
Conservative therapeutic measures
Conservative treatment should be performed depending on the respective phase of the disease. In Stage I, a potent anti-inflammatory therapy is indicated initially.
We treat, if no contraindication exists, with a single intra-articular injection of triamcinolone 40 mg, dexamethasone 8 mg to 10 ml bupivacaine 0.5%. Depending on the symptoms, a descending, oral prednisolone regimen of 30 mg, 20 mg, 10 mg prednisolone is additionally indicated every 10 days. Generally, the inflammatory stimulus is reduced rather quickly, so that after about 10 days, a gentle joint mobilization can be started. In addition to physiotherapy treatments, the patient is instructed to exercise according to an appropriate home exercise program in order to mobilize the glenohumeral joint several times a day.
Starting at Stage II, an intensified physiotherapy for passive mobilization of the glenohumeral joint in combination with manual therapy and metabolism activating action is recommended. Homeopathic and acupuncture treatments can accompany these measures if necessary. If, with the above measures after 3 to 4 months of therapy, there is no satisfactory improvement, arthroscopic capsulotomy and accompanying anesthetic mobilization are indicated.
Surgical therapy
Arthroscopic capsulotomy is an efficient and safe surgical technique for the treatment of persistent adhesive capsulitis of the shoulder. With a timely obtained diagnosis, the patient can be spared long and costly suffering.
In this procedure the rigid interval tissues is arthroscopically resected, ligaments glenohumeralia superior, medius and the inferior and the anterior and posterior capsule up to the caudal joint recess incised. The previously practiced sole mobilization under anesthesia should no longer be performed because of the associated risks and the poor treatment results.
The within the scope of the surgery inserted interscalene plexus should be left postoperatively to allow for a terminal passive motion therapy of at least 3 days under optimal elimination of pain. Physiotherapy should be continued on an outpatient basis with anti-inflammatory and analgesic medication.
Acromioclavicular joint arthrosis
Synonyms: acromioclavicular osteoarthritis, ACG osteoarthritis
Definition and Etiology
The acromioclavicular - (AC) joint is significantly involved in the power transmission between the upper limb and thorax. It is formed by the medial border of the acromion and the distal end of the clavicle. The articular disc is located between these two joint partners. Starting at age 20, it comes to degenerative changes of the fibrocartilage disc, which is ultimately the cause of early acromioclavicular joint arthrosis.
Due to the extreme mechanical stresses early osteoarthritis of the AC joint is a common disorder frequently found in athletes, especially if they participate in contact and power sports. Degenerative changes of acromioclavicular joint a common with age. However, these are often asymptomatic and only moderately correlated clinically.
Case history
The patient complains of pain in the most front, upper shoulder area, which under load, but frequently also occur after exposure. In particular, the lying on the shoulder is painful.
Clinical features
A therapeutic indicator is the clinical examination to distinguish symptomatic from asymptomatic acromioclavicular osteoarthritis. Typically for a symptomatic acromioclavicular joint osteoarthritis, is pressure pain over the often swollen AC joint.
Hyperabduktion and full flexion at AC joint are painful. In order to delimit differential diagnosis accompanying pathologies in the subacromial space or glenohumeral joint, a local infiltration test should be performed. A symptomatic affection of the acromioclavicular joint is indicated, if after intraarticular infiltration of 2 ml Buvivacain 0.5% previously positive tests are negative.
Imaging diagnostics
Radiology: Standard radiographs of the shoulder at three levels, as well as AC joint target images show a joint space of the acromioclavicular joint and osteophytes at the lateral clavicle. The radiological signs correlate only poorly with the clinical symptoms.
Ultrasound: Ultrasound often shows a narrowing of the joint space and joint effusion.
MRT: Magnetic resonance tomography exhibits a high sensitivity for the detection of early degenerative changes of the acromioclavicular joint, and especially a periarticular bone marrow edema or osteonecrosis of the lateral clavicle. Even secondary changes such as subacromial bursitis, subacromial impingement, tendonitis or rotator cuff tear, etc. can be detected.
Conservative therapy
The treatment of AC joint osteoarthritis is initially conservative. If rest, local anti-inflammatory drugs and cryotherapy do not results in significant improvement of the complaint symptoms, the local infiltration of acromioclavicular joint with dexamethasone 4 mg and 5 mg Triamchinon is indicated. If significant improvement is achieved, the treatment should possibly be continued with hyaluronic acid infiltration 3 to 5 times at weekly intervals
Surgical treatment
If conservative treatment measures fail, the goal of surgical treatment is to resect 8-10 mm bone from the lateral clavicle and thereby remove the painful contact of the bony joint partners. Arthroscopic resection of the lateral clavicle has been established as a standard procedure. The advantage here is that accompanying pathologies can also be treated minimally invasive.
Postoperative treatment
The treatment largely corresponds the of the subacromial decompression. The postoperative results are usually excellent, e.g. the patient can expect a painless and regain full arm and shoulder movement.
From the practice for the practice
The question here is HWS or shoulder
Of course, not all pain is based in the shoulder, radiating to the upper extremity pathology of the shoulder joint, frequently, it may also be the cervical spine that is responsible for a painful condition.
Formulated pragmatically, it comes down to the question: "How can I quickly and easily find out if changes in the shoulder or the cervical spine are the primary cause" Leading the way are, in our view, medical history notes and a simple preliminary investigation:
When asked, "Where does it hurt" we always ask the patient to show us the painful region since commonly the neck and shoulder region is referred to in the vernacular as “the shoulder”. If the patient points to the area of the trapezius or scapula, the probability is quite high that the complaints originate in the cervical spine and the muscles of the shoulder girdle. If the patient points to the shoulder joint or the deltoid, the main pathology is usually in the shoulder itself. An examination of the shoulder always includes exploratory study of the cervical spine. Reduced to a minimum is in our view the rule is: If passive movements of the cervical spine are painful, pathology of the cervical spine is the primary cause. If passive and active movements of the shoulder joint are painful, the primary pathology is expected to be in the shoulder.

PDF Download


