
Endoscopic Joint Replacement

PDF Download
Joint replacement - Hip – Knee – Shoulder
In Germany every year more than 400,000 people need an artificial joint. The endoprosthetic joint replacement is undoubtedly one of the most important surgical developments of the postwar period. Progress in both the design of joint prostheses as well as surgical techniques now allow for an individual treatment of osteoarthritis, tailored to the specific needs of the patient, with excellent results - particularly at the large joints. About 95 percent of the implanted prostheses last more than 10 years, 70-80 per cent more than 20 years. To promote scientific research, and to minimize the residual risk for complications to only 2 percent very low residual risk, an independent arthroplasty register should be started in Germany in the near future . Below, We would like to give a practice-oriented overview on the subject of arthroplasty of the large joints
Indications
The endoprosthetic joint replacement for osteoarthritis of the hip, knee and shoulder joint has increased steadily in Germany during recent years. Experts agree that the increase is certainly due to the demographic development in Germany, but is also a clear indicator of the performance of our health care system and its quality of care. To present the increase primarily as a pecuniary induced, uncritical obsession with surgeries, as it was propagandized very populist lately in the media, is certainly incorrect. Unfortunately, this confused many of the patients who would benefit from such an intervention.
Undoubtedly, to further improve the positive results after joint replacement, the indication for joint replacement must also be assessed critically in the future.
We must answer the patient's most important question: "When is the" right "time for joint replacement?". The essential factor here is the impact of osteoarthritis on the patient’s quality of life rather than the extent of osteoarthritis shown in the X-ray.
If conservative treatment measures do not benefit the patient sufficiently – even at the acceptance of minor complaints – to perform personally important tasks without major pain, a joint replacement surgery should be considered. The prerequisite is of course a corresponding finding, for example a radiological detection of advanced osteoarthritis that cannot be treated by a joint preserving surgical intervention. This applies even more, if the patient in addition to the stress pain also experiences pain during resting periods or at night and has to constantly rely on analgesics or anti-inflammatory agents. Of course, there are a number of factors influencing the decision for or against an endoprosthesis.
With an older, possibly polymorbid patient, surgical risk and "cost / benefit of the patient's perspective" must be weighed carefully against each other.
It is certainly true that being mobile and pain free is more important, the younger the patient. However, especially for very young patients, possibly limited durability of the prosthesis and the complexity of a possibly consecutively necessary prosthetic-change surgery must be taken into consideration. It should also be understood that after a joint replacement a return to high-performance-sports or even to stop-and-go sports such as soccer or other sports of this kind, is not likely to be recommended.
Extent of the osteoarthritis
Surgery should certainly not be performed only according to "X-ray” findings. However, it is important to not miss the right moment for an endoprosthetic joint replacement. If for example in progressive osteoarthritis the angular malalignment exceeds a certain degree, an axially supported endoprosthesis with a shorter life span must be implanted instead of a surface replacement. This applies also to other joints. If bony abrasion occurs, the anchoring of the prosthesis is difficult, resulting in a negative impact of function and durability. Determining the right timing for endoprosthetic joint replacement is an important medical task. A decision must be made on the basis of profound medical knowledge as well as being aware of the individual needs and expectations of the patient.
Hip hemiarthroplasty prosthesis
Hip implants are almost always implanted as total joint replacement if the patients are still very active. Hemiarthroplasty prosthesis involves only half of the hip (Hemi means half, not replacing the socket portion and arthroplasty means joint replacement.) and is indicated for older people who are typically less active, since it lowers the risk of the artificial femoral head to dislocate (protrusion).
The hip replacement was recently chosen by the scientific journal THE LANCET as "The Operation of the Century". Understandably so, because hardly any other surgery is so reliable and leads to full satisfaction of the patient
Shaft prostheses
Despite all the innovations regarding implant designs, innovations only work when linked to high standards. This is still the case with the classic shaft prosthesis, which achieves excellent long-term results and follow-up, often having a lifespan of more than 25 years
We distinguish between cementless anchored cemented prostheses, whereby their use mainly depends on the bone quality of the patient. Cement-free (titanium) implants are used in the harder bone of mostly younger patients and are "press-fit" anchored, resulting in a very high primary stability and usually allows immediate full weight bearing.
The cemented variant is often used for poor quality bone, such as in elderly people. The advantage is that the porous structure of the bone provides a larger anchoring surface and thus significantly lowers the risk of fracture at the insertion of the prosthesis
At the hip, head and socket allow for various materials, so called "pairings". Typical materials are ceramic, metal and polyethylene. In selecting the correct prosthesis for the patient, the surgeon has to weight the advantages and disadvantages according to clinical findings and the need of the patient.
Short-stem prostheses
A relatively new development is the group of short-stem prosthesis, which compared to the classic prostheses, are anchored in in the proximal and/or distal part of the femoral canal. The advantages of these implants are the bone-saving surgical technique at the femur and, if necessary, a less complicated prosthesis replacement surgery. Nothing changes for this type of prosthesis on the socket side. However, whether long term the rate of prosthesis loosening will come close to the established long-stem prosthesis, remains to be seen.
Cap prostheses
Some years ago, cap prostheses enjoyed a tremendous popularity because they were advertised as being extremely luxation safe and even more bone-saving than the short-stem prosthesis. The in many places fueled euphoria followed - unfortunately only with a few years delay - the disillusionment: squeaks and problems with metal abrasion due to metal-metal sliding pairing ( "The poisonous hip"), synovial tumors, femoral neck fractures and unnecessarily large bone loss on the problematic pan side because of excessive socket abrasion caused by the prespecified cap size. These disadvantages outweighed the benefits to the extent that the cap prosthesis today leads more or less a niche existence.
Minimally invasive surgical technique
One of the major innovations of recent years refers less to the implant itself as to the way it is introduced. Under the term minimally invasive surgery, various methods are subsumed, which all share tissue, in this case among other things muscle sparing and the relatively short incisions. Because of the reduced trauma to the musculoskeletal system, patients are able after the operation to complete the post-operative treatment faster and with less pain. The author of this article has personally great experience with the minimally invasive, anterolateral access according to Röttinger, which usually allows the patient to take the first steps after two days without crutches.
Luxation/dislocations
One of the most feared complications of hip arthroplasty is the luxation/dislocation. For this reason, the patients are given recommendations specifying which critical movements they should avoid temporarily. By using slightly larger head diameter, the replicability of the pre-existing neck-angle through the implant, optimum positioning of the implants and the preservation of muscle, the risk of dislocation is de facto today extremely low
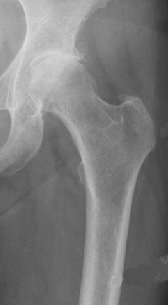
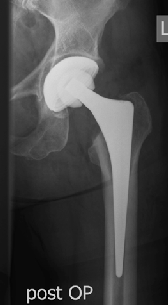
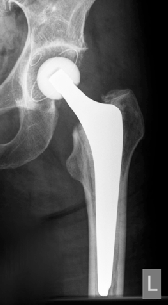
Coxarthrosis prae surgery-OP Hip-TEP cement free Hip-TEP cemented
Endoprosthesis Knee Joint
Mono / unicondylar knee prosthesis (Sled Prosthesis)
The classic indication for a monocondylar prosthetic knee, often called sliding prosthesis, is the unicompartmental wear of the joint, usually the medial compartment. The clinical results in lateral gonarthrosis are significantly worse due to the kinematics of the knee. If cartilage damage is also present in the other joint portion, the patient has an excessive deviation of the natural leg axis (genu varum), or if a higher grade ligament instability consist, a sled prosthesis should not be implanted. Minimally invasive techniques allow the implantation of prosthetic components with very little soft tissue trauma. As a rule, both the femoral and the tibial component are fixed with Palacos (bone cement). The unicompartmental sled influenced the kinematics of the knee joint only slightly. This enables early mobilization of the patient. The mobility is usually better than after conventional total knee arthroplasty. Overall, the implantation of a unicompartmental sled prosthesis is considered a very demanding operation, but shows excellent clinical results particularly with younger patients (55-65 years).
Bycondylar resurfacing
The principal indication for a bicondylar joint replacement is advanced joint degeneration, particularly if several joint compartments and sufficient ligament stability. Improvements in prosthetics design mean that in modern knee prosthesis as much of the natural structures is retained and only the worn articular surfaces are resurfaced. Because of the wide range of prosthetic models, such as gender specific models, individualized prostheses have not been successful. Due to the high primary stability and low rate of loosening, as a rule, both prosthesis components are cemented. After implantation of a knee prosthesis, the patient can expect a pain-free or at least pain-poor, good resilient knee joint in everyday life. In the first few months, there is often an increased feeling of tension, usually paired with an overheating of the joint. Frequently bending restriction remains with respect to the physiological flexion, which is seldom perceived as restrictive. The implant survival result after bicondylar resurfacing is about 20-years.
Axially supported knee endoprosthesis
If a sufficient ligament balance of the knee joint cannot be achieved by a resurfacing, an axially supported system must be used. This type of implant allows due to a more or less rigid coupling between the tibial and femoral component, the complete abandonment of ligamentous structures (collateral und cruciate ligaments). Compared to resurfacing, the more rigid the guide due to such a coupling, the more forces are transmitted to the components and their anchoring in the bone, which results in an overall higher rate of loosening and shorter implant survival time. Typical indications for an axially supported prosthetic arise primarily in the context of prostheses replacement operations or as a result of abrupt varus or valgus deformity. Since in both cases the patients are often older and consequently less active, meaning that they have limited functional demands with regard to a joint replacement, implantation of an axially supported knee endoprosthesis TEP can here prove very good solution..
Shoulder endoprosthesis
Thanks to the development of new types of prostheses and to improved design, shoulder arthroplasty has greatly advanced in recent years. Whereas in the past the clinical outcomes after joint replacement of the shoulder were rather moderate, they meanwhile show excellent results. The lifetime of shoulder prostheses are today approximately in the same range as those of the hip and knee replacement. High patient satisfaction is reflected among other things in the significant increase in numbers of operations. The range of indications for shoulder joint replacement ranges from classic omarthrosis to complex humeral fractures, posttraumatic caused joint defects, instability associated omarthrosis to rheumatic or tumorous articular defects. Depending on the indication, replacement is done with hemiarthroplasty, i.e. only the worn humeral head is replaced (total endoprosthesis), at which the head and socket, or an inverse endoprosthesis whose biomechanical principle is based on the articulation of a convex glenosphere with a concave joint partner at the humerus.
Hemiprosthesis
The indication for implantation of a shoulder hemiprothese, in which the humeral head is replaced without the joint socket, is advanced damage to the humeral head and relatively good socket conditions, e.g. in a necrosis of the humeral head, an early stage of osteoarthritis without a decentration of the humeral head, or unsuccessfully healed humeral head frakture.
Cap prosthesis
The cap prosthesis is a pure surface replacement of the humeral head, in which the worn joint surface is crowned with a metal cap. The advantage of this pure "resurfacing" is that a maximum amount of autogenous bone is left, which is ideal for possible future revision. The anchoring of this prosthesis is usually performed cementless. Although, the name is close to the cap prosthesis at the hip, it is a completely different principle that pursues the high-problematic metal on metal sliding. Shoulders that achieve a good centering after implantation of this type of prosthesis often show with this most defense type of all shoulder prostheses permanently very good functional results.
Hemiprosthesis stemless shoulder prosthesis
Just like with a stem prosthesis, the stemless hemiprosthesis is implanted to resection the head at the level of the anatomic neck, whereby the anchoring of the new head does not take place with the stem in the shaft, but only in the epiphysis, the most proximal part of the humerus. Advantages of this method are the anatomical reconstruction of the original joint kinematics and the good easy removal in the event of a revision. The stemless prosthesis is also implantable as arthroplasty, meaning with simultaneous socket replacement. Important for the implantation of such prosthesis is a good bone quality in the proximal humerus. Currently loosening rates do not differ from those of the classic stem prostheses
Stem prosthesis
The indication for a stem prosthesis as a hemiprosthesis, is given in cases where due to poor bone quality or in the context of fractures a head prosthesis cannot be anchored with primary stability. Thus, this type of prosthesis, which was almost exclusively used at the beginning of shoulder arthroplasty, is today rarely used.
Total endoprosthesis
A total endoprosthesis replaces the joint surface at the glenoid. In recent years, there is a clear trend towards socket replacement because in situations with significant socket wear, a total endoprosthesis achieves an even better functional result than is the case with hemiprosthesis. Since the implanted socket shows loosening slightly earlier than the head components, total endoprosthesis are used more the elderly patients. If the osteoarthritis is present over a longer period, it may lead to a more or less distinct dorsal abrasion of the acetabulum with consecutive dorsal subluxation of the humeral head. This form of osteoarthritis is called eccentric osteoarthritis. In the presence of eccentric omarthrosis implanting an endoprosthesis is always an indication for the joint to "re-center" again.
Anatomic total endoprosthesis
In case of an intact rotator cuff, so- called anatomic implants are inserted. The shoulder prosthesis now in its fourth generation can mimic the original joint anatomy with its modularity perfectly and allows for a change of worn components. The design of the new joint socket has changed significantly compared to previous generations. Earlier generations had the same radius of curvature as the prosthetic head. By eccentric stress on the glenoid there were frequently premature socket loosenings ( "Rocking Horse" phenomenon). To avoid eccentric loads, joint sockets have been developed, whose radius is larger than the matching prosthetic head (what we call a "mismatch"). Studies show that total endoprostheses provide excellent results with respect to the function and the pain.
Inverse shoulder prosthesis
Inverse shoulder prosthesis, developed in the '80s, show a reversal of the normal anatomic conditions. Instead of a convex humeral head, the inverse shoulder prosthesis at the upper arm has a concave shape, and instead of a concave socket at the glenoid, it has an approximately hemispherical shape (glenosphere). Because of this reversal, the center of rotation of the joint is medially displaced and the power is transmitted almost exclusively through the deltoid muscle (see diagram below). Accordingly, the main indication represents the advanced arthropathy with irreparable rotator cuff tear. In recent years, the inverse prostheses have become the fastest developing segment for shoulder replacements. Despite many concerns, the reason is an excellent 10-year result now evidenced in studies. Technical innovations result in good to excellent clinical results, meaning they achieve very good pain relief and good functional improvement. This is true in particular in cases where previously a hemiarthroplasty or anatomical shoulder prosthesis could only achieve poor results. The design improvements of the inverse prosthesis and correction of the previously critical "notching" phenomenon also result in a lower loosening and revision rate.
From the practice for the practice
Endoprosthese and Sports – what is allowed, what is not allowed?
Due to increasingly improved clinical results after joint replacement and a growing demand of our patients to remain active even in a mature age, physicians are more often asked, "Can I participate in sports with my prosthesis?" The following facts may help you, to answer the question reliably.
Shoulder prosthesis
In various everyday movements and activities the forces acting in the shoulder joint, are comparatively low. The maximum compressive force in the shoulder joint during daily activities is about 0.5 times body weight. In contrast, when walking down stairs forces are mobilized in the knee joints that equal 6 to 8 time’s standard body weight. Nevertheless, patients should be advised to be more cautious with shoulder stressful sports after shoulder endoprosthesis. Despite the improved biomechanical and tribological properties of modern prostheses, too intense physical stress can in particular lead to premature loosening of the glenoid component lead.
The American Society for Shoulder and Elbow Surgery recommends sports with low load on the upper extremity and low accident risk. This includes jogging, swimming, cycling, bowling, dancing and low-impact aerobics or gymnastics. Allowed is also skiing and golf, if previous experiences already exist in this sport. Not recommended are tennis and volleyball. Jensen and Rockwood studied 24 patients who were playing golf preoperatively, and found that after implantation of a shoulder endoprosthesis more than 90% of the patients could play golf again after an average of 4.5 months at the same level as before. In some cases, the handicap was even reduced. Radiologically there was no increased rate of loosening. (J Shoulder Elbow Surg)
Knee prosthesis
More than with other prostheses after implantation of a knee endoprosthesis often a considerable functional deficit remains. The expectations of the patient to achieve a given level of performance after the operation must be put into perspective. Limiting factors are among others, the often limited flexion, loss of proprioception, changes in the ligaments, and poorer muscular coordination.
Consequently, for ambitious patients specific strategies are essential to avoid overloading the polyethylene with increased wear or loosening of the implant bone connection: the patient may not resume sporting activities until at least 6 months postoperatively. Primarily the patients should participate in sports participated in before the surgery, especially for the knee joint complex loads. The frequency of sports training is to be adapted to the reduced capacity of the artificial joint.
Unobjectionable activities and sports
Walking, cycling, swimming (breaststroke should be avoided), hiking (avoid walking downhill or use walking sticks), Nordic walking, and golf, boating.
Sports recommended, however, with some restrictions
Jogging (only on soft elastic substrate with optimal footwear, short stride), cross-country skiing (without steep descents, no skating), fitness training, gymnastics, dance, tennis (with reduced ambition rather double than single, sand or granular soil, no non-slip floor coverings).
Sports not recommended
Sports with a high risk of injury (combat and contact sports) or high risk of falling (Alpine skiing, rollerblading or ice skating), football, volleyball, handball, and other stop-and-go sports.
Hip prosthesis
After implantation of a hip prosthesis, most patients return very quickly to a previously unthinkable level of activity in everyday life. However, persons who are active in sports, frequently ask after 2-3 months when they can possible resume their sports activities.
Recommended sports do not differ fundamentally from those, which are possible with a knee endoprosthesis (s. above).
The date of returning to sports depends essentially on two factors:
Firstly, it can be assumed is that in the first 3-6 months after surgery a neo-capsule will form around the joint. Consequently, special attention must be paid to the type of movements or activities, e.g. during this time, swinging movements in the luxation-critical movement direction as for example, in gymnastic exercises should be avoided.
Secondly, it is important to also take the joints guiding and pelvic-stabilizing muscles, which may be affected to differing degrees before surgery. Here, minimally invasive surgical techniques are very beneficial. Movements that are performed with dormant or uncoordinated muscles strain prosthesis excessively. Therefore, a specific compensation of such deficits is important prior to starting a sport specific training.

PDF Download


