Joint Replacement Knee
What does "artificial knee joint" or knee arthroplasty mean?
There is not the just the one "artificial knee joint"; rather, there are a number of different ways to treat the worn joint surfaces of the knee with artificial implants. Depending on the extent and the location of the damage, completely different implants are being used to restore the function of the joint.
Today, the most important goal is to only replace the worn portions of the joint and to preserve as much of the healthy body tissue as possible.
To understand the different treatment concepts, it must be kept in mind that the knee joint is composed of three different joint parts: one located in each case at the inside and the outside of the joint portion between the thigh and the lower leg as well as the joint portion between the knee cap and the femur.
The basic options of knee joint replacement are:
Partial joint replacement (PKR) / sled prosthesis
If only a certain part of the knee is worn out and the other parts of joint are in a good condition, it may be appropriate to only replace the worn part with a new joint surface. Such a procedure is called partial joint replacement or "sled prosthesis".
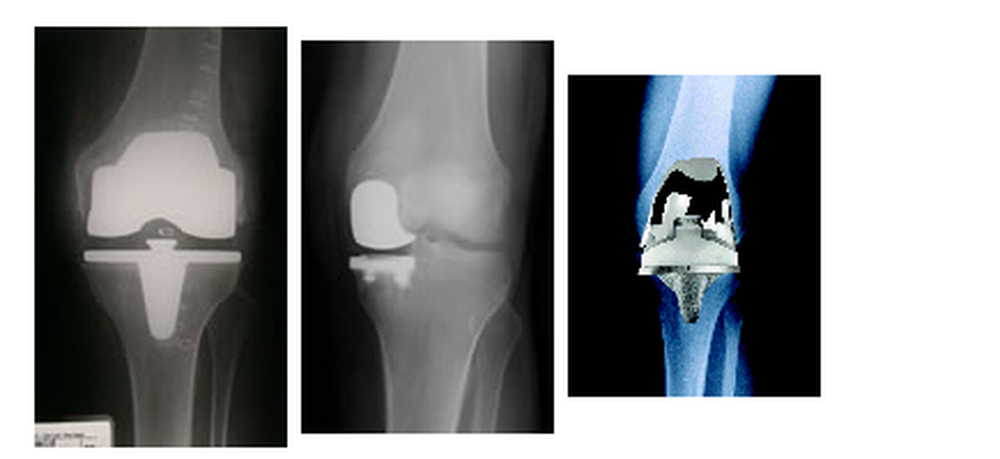
Complete surface replacement (TKR) / bicondylar surface replacement
If more than one section of the knee joint is heavily worn, all elements of the joint should be resurfaced, meaning they should be crowned with a metal cap. Thus the ligament structures essential for the stabilization of the joint are preserved. This type of knee replacement is called "complete" or in medical terms “bicondylar” surface replacement".
Axially supported knee endoprosthesis
If, in the context of progressive osteoarthritis, a marked deformity of the knee (O-leg or X-leg position) has developed, it will not suffice to only crown the worn joint surfaces. In such cases, the no longer functional guiding ligaments of the knee joint must be replaced. This is done with a more complex implant, a so-called axially supported endoprosthesis.
All the joint replacements described above, have in common that the new joint surfaces are made of metal alloys (titanium or cobalt-chromium-molybdenum alloy). A sliding surface of special plastic polymers imitating the human lubricative cartilage layer, is inserted between these metal surfaces. The metal joint surfaces are, almost without exception, fixed directly on the prepared joint ends of the upper and lower leg bone with a two-component glue, the so-called bone cement. A cementless anchorage, as known in a hip of the shoulder joint replacement, is due to the anatomical conditions an exception.
When does a knee joint replacement (endoprosthesis) make sense?
Resurfacing the worn joint surfaces, or how is commonly referred to replacing the knee joint with an endoprosthesis, should be a serious consideration when despite a treatment of degenerative knee arthritis (see joint degeneration / osteoarthritis) the quality of life of the patient is permanently affected by severe pain.
With more than one hundred thousand cases per year, the artificial replacement of the knee joint is one of the most often performed orthopedic surgeries in Germany.
Timing is a crucial factor when replacing or resurfacing a knee joint. Although, the artificial joint replacement does improve the quality of life and mobility of the patient significantly, the durability of an artificial joint is limited. It is therefore essential to also take the patient's age into consideration when deciding for this type of procedure. The durability of an artificial knee joint is statistically between 15-25 years. However, after this period, a replacement of the prosthesis is in most cases possible.
However, it is also essential to consider that it is definitely advisable to replace a worn knee joint surface in a timely manner rather than to wait until a more complex axially-supported endoprosthesis becomes necessary due to increasing wear, e.g. advanced degenerative osteoarthritis.
 Video: Kniegelenk Arthrose TEP OP
Video: Kniegelenk Arthrose TEP OP
What are the risks of a knee joint replacement surgery?
As with any medical procedure, there are risks that must be considered prior to surgery. Some of the overall risks are general risks, meaning complications commonly occurring and restricting the hoped for success of the surgery.
Common surgery-related risks are infections, wound healing, or thrombosis. The risk of an operation and what can be done to minimize those risks should be thoroughly discussed with the surgeon prior to the procedures. Additional risk factors are diseases the patient might have prior to surgery and/or his or her physical condition. These risks need to be considered and discussed with the surgeon prior to the surgery. Additionally there may be risks due to internal diseases. These types of risks should also be discussed in depth with the surgeon and the anesthesiologist.
What type of anesthesia is required prior to a joint replacement surgery of the knee?
In most cases, general anesthesia is administered approximately 1.5 to 2 hours prior to the replacement surgery of the knee. Due to the medical, technical and pharmacological progress in recent years, general anesthesia is generally well tolerated.
General anesthesia is often combined with local anesthetics of the nerves that supply the knee joint. That means that even less medication is needed for general anesthesia and that it is even better tolerated by the patient. However, such a decision should only be made on a case to case basis after an appropriate examination of the patient by the anesthetist. Any post-operative pain is due to improved anesthetic procedures and appropriate pain medication usually is not very strong.
What treatment is necessary after a knee joint replacement surgery?
Early mobilization is important. Already on the first day after the operation the patient will start the first walking exercise. During the first two weeks, crutches are recommended.
A targeted physiotherapy will support the healing process. A hospital stay of about one week should be expected. Further rehabilitation either takes place during an approximate 3-week stay in an appropriate rehabilitation center or on an outpatient basis. Continuation of physiotherapy treatments should be considered case by case. With a normal every day stress level, full mobility is generally obtained after a few weeks. Whether the patient can participate in sports with the artificial knee joint must be discussed with the treating physician.
Specialists: Artificial Knee Joint
For an optimal treatment of a degenerative arthritis/osteoarthritis, the knee and shoulder experts at the Klinik am Ring are particularly well-qualified. Stefan Preis, M.D. and Jörg Schroeder, M.D., senior physicians at the Practice and Department of Orthopedics and Sports Traumatology at the Klinik am Ring in Cologne, specialize together with their team in the treatment of knee and shoulder disorders. In 2004, they founded the WEST GERMAN SHOULDER KNEE & CENTER, Cologne. The team consisting of eight specialists treats more than 10,000 patients annually. Per year, they are conducting more than 1,200 partially very complex operations on the knee.



